Watch live
Monday to Friday
In Case You Missed It
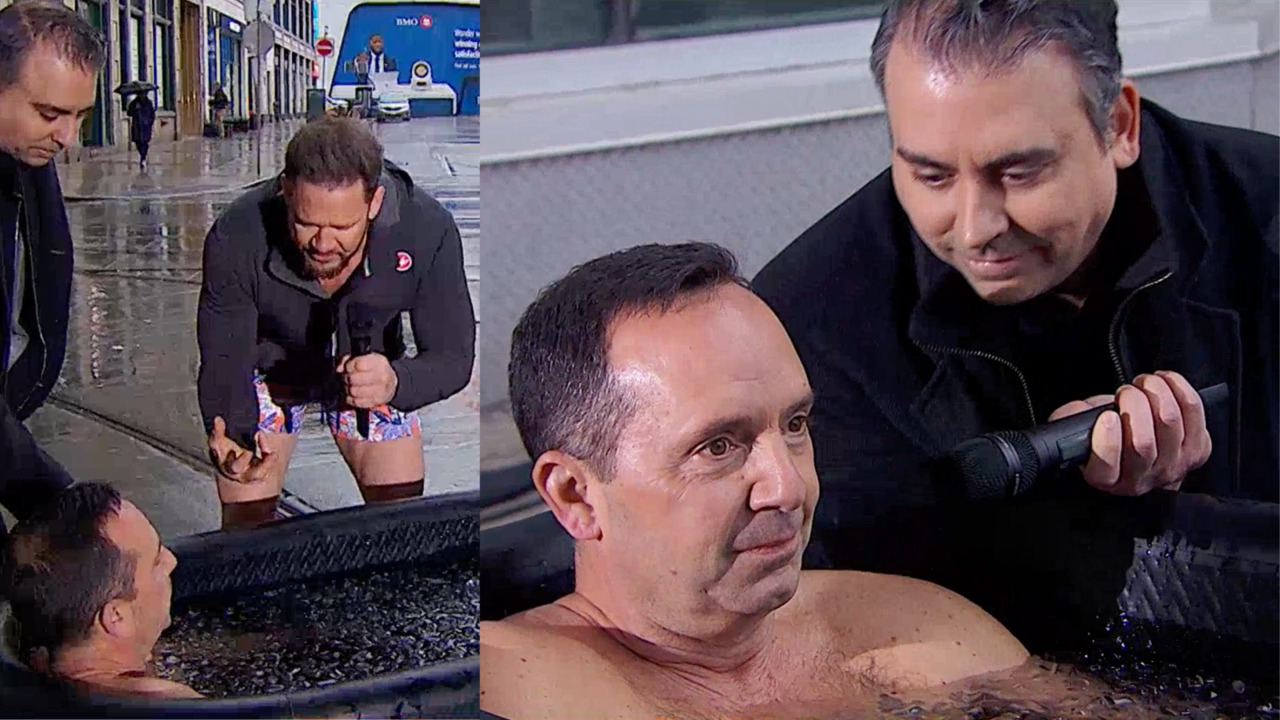
Weatherman Frankie Flowers does a cold plunge LIVE on national television
Celebrate with BT

Connect with @breakfasttelevision
live, weekday mornings
Subscribe or follow to watch live weekday mornings on Citytv, YouTube and Facebook. Connect with us on Instagram and Twitter for more news and entertainment